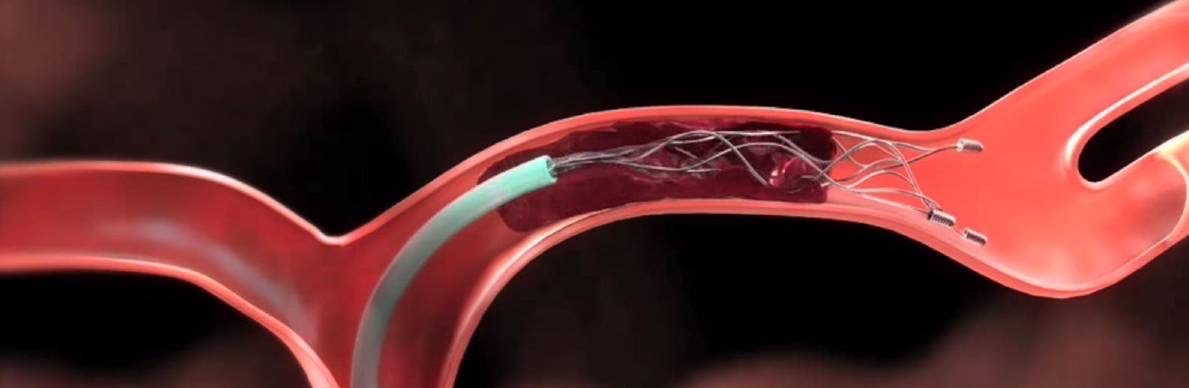
Thrombectomy: A Revolution in Stroke Care
The pictures that adorned the walls of her nursing home room captured the spirit of a vibrant young lady with a true zest for life. Joyful images of hiking adventures, bike rides, and stunning mountain vistas painted a picture of someone full of energy. Yet, this woman seemed unfamiliar to me in her current state.
As a college student working part-time as a nursing assistant, I got to know her very well. While she was always kind and pleasant, a deep sadness lingered around her, and I often found her in tears alone in her room.
But why should that have surprised me? After all, she couldn’t move the right side of her body after suffering an acute ischemic stroke (AIS) just two years earlier when she was only 61 years old. A tiny clot had stolen her ability to move and care for herself by blocking a blood vessel in her brain.
Regrettably, stories like hers are all too familiar, both in the U.S. and around the globe.
An AIS occurs when a brain vessel becomes blocked, denying brain tissue the oxygen and nutrients it needs to survive. Most commonly, this blockage is caused by a blood clot—an embolus—that gets stuck in a vessel. An AIS can have devastating consequences depending on which brain area is affected. Many individuals who experience an AIS might lose their ability to move specific body parts, like an arm or a leg, while others could suffer vision loss. Some might even struggle with moving their facial muscles or swallowing food.
Brain cells are uniquely susceptible to a lack of blood flow and can die quickly when this supply is cut off. That’s why prompt emergency care is essential for patients suspected of having an AIS. “Time is brain” is a crucial reminder of the urgency here.
A Persistent Problem with Limited Options
The impact of strokes has been felt throughout history, with ancient physicians identifying symptoms of an AIS, like sudden arm or leg paralysis, even without modern imaging tools like a CT or MRI scan. Although we've come a long way in diagnostic accuracy, treatment options have been limited for centuries. Renowned Greek physician Galen wisely noted that the best way to address a stroke is to prevent it from occurring in the first place—a principle that is just as relevant today.
Recent advances in medical imaging have allowed doctors to diagnose strokes more accurately. However, even with improved diagnostics, treatment options have not kept pace. It's frustrating to consider an enhanced ability to recognize stroke without equally effective treatments available.
Fortunately, a landmark moment occurred in the 1970s when Belgian biologist Désiré Collen introduced tissue plasminogen activator (t-PA). This drug that can dissolve clots blocking blood flow to the brain and has been most commonly administered through an intravenous (IV) injection. A pivotal clinical trial in 1995 showcased the benefits of t-PA for patients with AIS, igniting global interest in stroke and stroke research. An important lesson was learned from this study: promptly clearing blockages leads to better outcomes.
t-PA received approval for human use in 1996. But even with proven efficacy, it was often wondered if there is room for improvement.
Without a doubt, t-PA has been a groundbreaking advancement and has helped save millions of lives, preventing death or permanent disability. However, the use of t-PA comes with restrictions. For example, patients suspected of having an AIS who have had one in the past—which is not uncommon—might not be eligible for t-PA due to the risk of bleeding in the brain. Moreover, t-PA is generally reserved for patients who arrive at the hospital within 4.5 hours of experiencing their first stroke symptoms, meaning that patients who come to the emergency room later than that may not receive a benefit. It may also be ineffective against dense clots obstructing larger brain vessels.
Given these restrictions, the quest for developing new stroke treatments beyond t-PA remained an important focus.
Into the Artery: Intra-arterial t-PA and Mechanical Thrombectomy
Historically, t-PA has been given to patients by injecting it into a vein, most commonly in the arm. Could there be a better way to administer t-PA to a patient? Spurred by advances in imaging, interventional radiologists in the 1980s and 90s wondered if giving t-PA directly to the clot—by directing a tiny catheter through the groin and up into the blocked blood vessel in the brain—would lead to better outcomes. This approach is referred to as intra-arterial tPA or intra-arterial thrombolysis.
Two clinical trials demonstrated a modest benefit of intra-arterial t-PA, but this came with a cost: An increased risk of bleeding in the brain was found in patients who received intra-arterial t-PA. Although a solid scientific concept, the results of these studies were disappointing.
However, a more revolutionary idea was born from these studies: guiding a small catheter into the blocked vessel in the brain could be used to access the clot directly. Could it be mechanically removed from the vessel instead of trying to dissolve the clot with a medication? After all, it was known that restoring blood flow in the blocked vessel was the primary goal for stroke treatment. This thought spurred several medical device companies to develop small catheters that utilize a stent—or stent retrievers— that could remove a clot obstructing a large artery in the brain. This approach—referred to as mechanical thrombectomy (MT)—was of interest to doctors throughout the globe.
Though stent retrievers effectively removed clots from large arteries, a series of studies in the early 2000s failed to demonstrate any meaningful clinical benefit in patients treated with MT versus t-PA alone. However, doctors had many concerns about these studies and their results. For example, many patients were included in the study who already had large areas of brain death from an AIS, meaning that restoring flow would not benefit such patients. For these reasons, researchers and doctors around the globe continued, nevertheless, to question if MT could provide a benefit for patients with AIS.
The hope of MT as a beneficial therapy for AIS was still strong.
An Obvious Benefit
Stroke doctors will forever remember 2015, when five large, well-designed clinical studies were published in the New England Journal of Medicine. Each of these studies consistently demonstrated the benefit of MT in patients suffering from an AIS. Of equal importance, study doctors did not find an increased risk of brain bleeding in MT patients.
The effect of MT was so prominent and overwhelming that four studies were terminated early.
Just how influential was MT in these studies? Data from the five trials found that the number needed to treat (NNT)—a measurement of treatment effectiveness where the lower the number, the better—was 2.6. This means that roughly three patients with a stroke need to be treated with MT to improve one patient’s function.
To compare, Aspirin—a commonly prescribed drug for heart attack prevention—has an estimated NNT ranging from 50 to 360. This means that 50 to 360 patients need to take aspirin for a single heart attack to be prevented in one patient. This puts the astounding data from these five stroke studies into an accurate context.
These studies also demonstrated that all categories of patients treated with MT benefited from it—regardless of age, sex, clot site, or symptom severity. This means that MT can be used across a broad range of patients and is not restrictive to specific patient subgroups, unlike t-PA.
Here is more information on the data from these monumental studies.
Mechanical thrombectomy was rightfully catapulted to the front of the treatment line for patients with AIS caused by large occlusions of a brain vessel.
New Innovations and Future Directions
The 2015 data were significant, consistent, and astounding to stroke clinicians. Accordingly, an explosion of technology occurred after these data were published.
But could we treat stroke patients even better? Despite the obvious clinical benefit of MT from the 2015 studies, there was room for improvement. For example, complete removal of the clot only happened in 50 to 70% of patients, and, as we now understand, complete restoration of blood flow is the key to the best outcomes.
Several questions permeated the minds of doctors and researchers, paving the way for several advances after 2015.
Is the stent retriever the best way to get the clot out? Could it be “sucked” out instead? This thought led to the development of aspiration catheters, which, instead of using a stent to remove the clot, used suction to take the clot out of the vessel. To this day, however, it remains unclear which device—aspiration catheters or stent retrievers—removes clots more effectively.
Can we prevent debris from other blood vessels—such as the carotid artery, when guiding the catheter into the brain—from lodging into other, smaller vessels in the brain? Or, can we change the direction of blood flow in the brain vessels to improve our ability to remove the clot? This idea led to the development of catheters with balloons— balloon guide catheters— which could be inflated in the carotid artery in the neck. The inflated balloon could block debris from entering the brain while, at the same time, changing the blood flow direction in the brain to help move the clot out of the vessel. The development of balloon guide catheters has further improved outcomes for stroke patients treated with MT.
Beyond devices, patient selection criteria for MT have expanded; additional clinical studies have shown that patients who arrive at the hospital outside the treatment window—typically 6 hours—can also benefit from MT.
Other questions remain, which, when answered, could provide additional benefits for patients with AIS. Can we use advanced imaging to better select patients with AIS who may benefit from MT? Can patients benefit from MT at much later time points? Can smaller devices remove clots in tiny vessels and other brain areas? Can we develop better medications to dissolve clots to use alongside MT devices?
A New Horizon
When reading about all of the new advancements in MT and stroke care, I wonder what would have happened if my nursing home patient had a stroke a few years later—after the explosion of clinical data and the development of advanced MT technology. Perhaps I wouldn’t have met her in the first place, as she might have been saved from her devastating disability.
It's disheartening to think of the millions of patients living with a permanent disability who suffered a stroke before 2015. Without a doubt, this number would be far smaller if the MT explosion had occurred earlier. Unfortunately, acute ischemic stroke remains common, disabling, expensive, and potentially deadly.
In contrast to Galen's time, however, there is now an apparent global interest in advancing stroke care and research, and the MT paradigm continues. Thanks to the MT revolution and those who made it happen, the future of care for AIS is remarkably bright.
For a Deeper Dive
t-PA
https://karger.com/ced/article/50/6/666/821945
https://www.ahajournals.org/doi/full/10.1161/STROKEAHA.114.007564
https://jamanetwork.com/journals/jama/fullarticle/192156#google_vignette
https://www.nejm.org/doi/full/10.1056/NEJM199512143332401
https://www.amazon.com/tPA-Stroke-Story-Controversial-Drug/dp/0195393929
Mechanical Thrombectomy
https://www.thelancet.com/journals/lancet/article/PIIS0140-6736(16)00163-X/abstract
https://link.springer.com/article/10.1007/s11940-024-00796-5
New Advances and Future Directions
https://www.thelancet.com/journals/lancet/article/PIIS0140-6736(19)30297-1/abstract
https://jamanetwork.com/journals/jama/fullarticle/2784507
https://jamanetwork.com/journals/jama/fullarticle/2784507
https://www.nejm.org/doi/full/10.1056/NEJMoa1706442
https://www.nejm.org/doi/full/10.1056/NEJMoa1713973
https://jnis.bmj.com/content/10/4/335
https://link.springer.com/article/10.1007/s11940-024-00796-5

Post a comment