
Pulsed Field Ablation and Why it Matters for Medical Writers
I remember meeting a miserable man as a medical student during my emergency medicine rotation. He lay on a rickety bed with light blue sheets that were darkened with sweat dripping from his thin body. Breathing rapidly, he kept his eyes closed and his teeth clenched, his left hand rested over his eyes in a futile attempt to soothe his nausea. “I feel like a stampede is running through my chest,” he said hoarsely.
He was in atrial fibrillation (AF)—an irregular rhythm of the heart's upper chambers, anatomically referred to as the atria.
Patients with AF—like this unfortunate fellow—often experience such symptoms. More insidiously than these symptoms, AF increases the risk of ischemic stroke: When blood remains stagnant in the fibrillating atria, clots can form and may be catapulted up into the carotid and more distal arterial network of the brain, leading to an ischemic stroke.
Patients with AF are often treated with blood-thinning medications to prevent clots from forming. While newer blood thinners have improved upon their predecessor—warfarin, an antiquated drug that significantly increases the risk of bleeding in other areas of the body—they are not without their risks. Moreover, medications intended to prevent the abnormal rhythms of AF from occurring don’t always work.
Clinicians and researchers have long recognized the need for alternative options.
In 1998, Dr. Michel Haïssaguerre, a French electrophysiologist, published a seminal paper in the New England Journal of Medicine detailing his use of radiofrequency ablation (RFA)—specifically, the application of extreme heat to heart tissue via a small catheter—to disrupt the pathway of abnormal electrical signals in the heart that cause AF.1 By maneuvering a small catheter from the femoral artery into the left atrium with image guidance, Haïssaguerre successfully mapped the origins of these errant electrical signals—most commonly from the pulmonary vein, a large vessel that transports oxygenated blood from the lungs to the heart—and utilized RFA to intentionally eliminate the heart cells responsible for transmitting the divergent electrical signals from the pulmonary vein into the atria. This procedure, known as pulmonary vein isolation (PVI), has since become a standard treatment for AF that cannot be effectively managed with medication alone.
Although Dr. Haïssaguerre was not the first to employ RFA for treating abnormal heart rhythms, his early work established a foundation for future catheter-based interventions for treating AF.2 Since Dr. Haïssaguerre’s initial research, catheter-based PVI procedures have continued to evolve. Safer, sleeker, and more navigable catheter systems have been developed, and more sophisticated electrical mapping techniques are now used.
Additionally, cryoablation—using extreme cold to ablate heart tissue—has been developed as an alternative to RFA for PVI.3 Despite the effectiveness of RFA and cryoablation in treating AF, these thermal methods have several downsides, including lengthy procedure times and risks of tissue damage, such as perforation of the heart wall or injury to nearby structures like the esophagus or phrenic nerve.
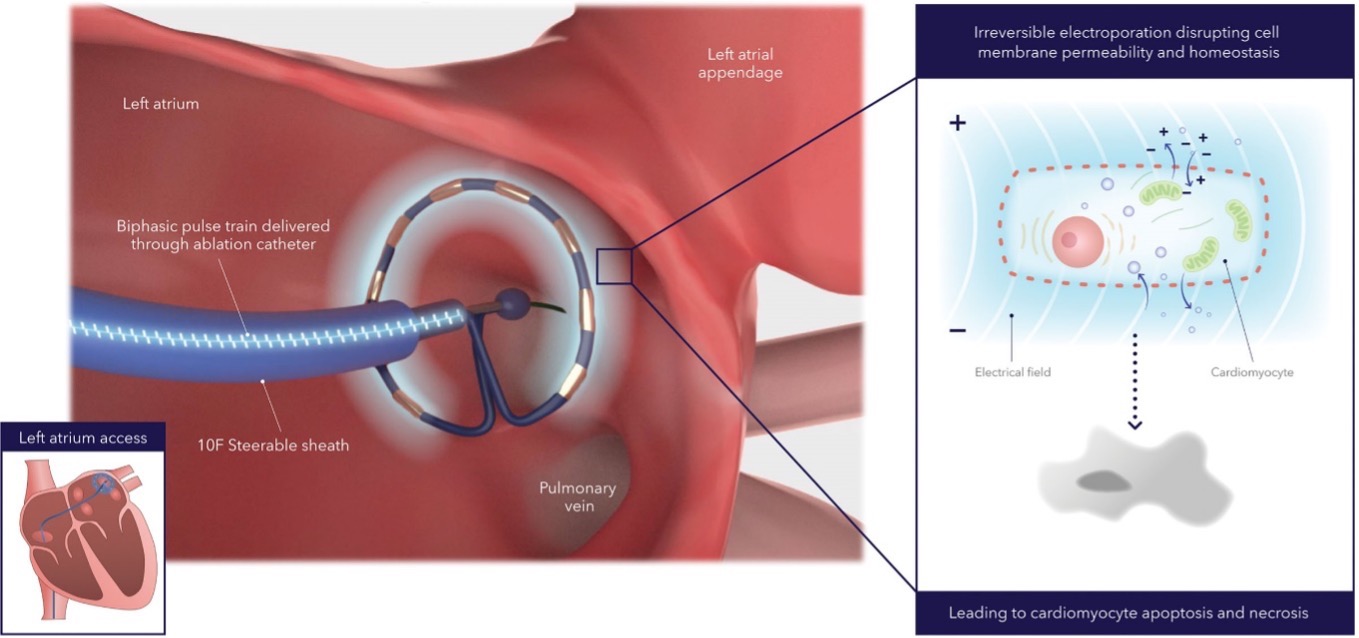
These challenges posed by thermal-based ablation procedures prompted cardiologists and researchers to explore alternative solutions. In the early 2010s, clinicians and scientists began investigating pulsed-field ablation (PFA), which uses non-thermal electroporation—rapid electrical signals that punch tiny openings in the membranes of heart cells, leading to their demise. I’ve included Figure 1 from a recent clinical trial to illustrate this. Compared to thermal ablation methods, PFA was believed to ablate cardiac tissue more precisely and in less time, which may, in theory, lead to improved safety and reduced procedure times.
Indeed, since 2018, several clinical studies—both observational and randomized trials—have shown that PFA seems to have a better safety profile and shorter procedure times compared to thermal-based methods.4 Along with low rates of adverse events, other early trials indicate that PFA seems to be at least non-inferior to thermal-based methods regarding procedural success and short-term control of AF.5,6 Recently, in July 2024, results from the MANIFEST 17K study—a multicenter retrospective safety analysis involving over 17,000 patients across 106 sites treated with Boston Scientific’s FARAPULSE PFA system—revealed exceptionally low adverse event rates, indicating that PFA has an improved safety profile compared to thermal-based methods.7
Despite this promising data, many questions remain: Is PFA superior to thermal ablation in direct trials? Are the safety and effectiveness profiles demonstrated in long-term follow-up studies? Are certain PFA systems more effective than others? Is it cost-effective? How can we enhance PFA technology further? Given these questions, several clinical trials are underway. Although more data are needed, many leaders in the interventional cardiology field have noted that this technology signifies a remarkable advancement in AF treatment.7,8
Why is PFA important to medical writers? As Mark Twain famously said, “Write what you know,” and many medical writers will inevitably write about PFA at some point.
Regardless of niche, medical writers operate at the cutting edge of medical science. Indeed, PFA signifies a major advancement in the cardiac arena and is expected to keep growing; the PFA market surpassed $500 million in 2024, and due to its success in recent trials, many experts predict that the PFA market will continue expanding at this rapid pace.
Suppose you are seeking a role in regulatory writing. In that case, many device giants in the cardiac ablation space (including Boston Scientific and Medtronic) are expanding their cardiac ablation portfolios, likely including newer PFA devices. Consequently, these devices will need regulatory approval in the U.S., E.U., and other international jurisdictions. With the PFA market projected to grow, other device companies (such as Johnson and Johnson) will likely look to establish a market presence in this area as well. It’s possible, then, that much of your work in these settings will focus on interpreting and communicating clinical data related to your company’s PFA products as part of a clinical evaluation report, say. It is, therefore, important to understand what PFA entails and its successes in clinical studies thus far.
Other areas of medical writing will undoubtedly engage with PFA technology. Device company sponsors are certainly looking to fund continuing medical education (CME) activities that center on PFA—and perhaps not unintentionally, their product—indicating that CME writers who create gap analyses and needs assessments will need to explore the PFA literature.
There are many other examples of how medical writers must engage with PFA. However, PFA will undoubtedly remain a dominant technology in the cardiac ablation space for years to come. Medical writers will benefit from understanding how it works and the clinical data supporting its use.
References
1. Haissaguerre M, Jaïs P, Shah DC, et al. Spontaneous initiation of atrial fibrillation by ectopic beats originating in the pulmonary veins. New England Journal of Medicine. 1998;339(10):659-666.
2. Scheinman MM, Morady F, Hess DS, Gonzalez R. Catheter-induced ablation of the atrioventricular junction to control refractory supraventricular arrhythmias. Jama. 1982;248(7):851-855.
3. Packer DL, Kowal RC, Wheelan KR, et al. Cryoballoon ablation of pulmonary veins for paroxysmal atrial fibrillation: first results of the North American Arctic Front (STOP AF) pivotal trial. Journal of the American College of Cardiology. 2013;61(16):1713-1723.
4. Reddy VY, Koruth J, Jais P, et al. Ablation of atrial fibrillation with pulsed electric fields: an ultra-rapid, tissue-selective modality for cardiac ablation. JACC: Clinical Electrophysiology. 2018;4(8):987-995.
5. Reddy VY, Gerstenfeld EP, Natale A, et al. Pulsed field or conventional thermal ablation for paroxysmal atrial fibrillation. New England Journal of Medicine. 2023;389(18):1660-1671.
6. Verma A, Haines DE, Boersma LV, et al. Pulsed field ablation for the treatment of atrial fibrillation: PULSED AF pivotal trial. Circulation. 2023;147(19):1422-1432.
7. Ekanem E, Neuzil P, Reichlin T, et al. Safety of pulsed field ablation in more than 17,000 patients with atrial fibrillation in the MANIFEST-17K study. Nature medicine. 2024;30(7):2020-2029.
8. Russo AM. Pulsed field ablation: is it better than conventional thermal ablation for treatment of atrial fibrillation? : Lippincott Williams & Wilkins Hagerstown, MD; 2023. p. 1433-1435.

Post a comment